Stevens-Johnson Syndrome
Stevens-Johnson syndrome is an immune-complex-mediated hypersensitivity complex.
It is a variant of bullous erythema
multiforme. It ranges from mild skin and mucous membrane lesions to a severe,
sometimes fatal systemic disorder. Ocular symptoms include ulcerative
conjunctivitis,
keratitis,
iritis, uveitis,
and sometimes
blindness.
Epidemiology
- More common in Caucasians
- More common in males than females
- Most patients are aged 10-30 but cases have been reported in children as young as
3 months
- Tends to be more common in winter and early spring
Risk Factors
- Past history of Stevens-Johnson syndrome or erythema multiforme
- Recurrences may occur if the responsible agent is not eliminated or if there is
a further exposure (e.g. drug).
Causes
The most common causes in adults are drugs and malignancies. In children, the most
common causes are infections.
Infection
- Viral: includes
herpes simplex virus,
Epstein-Barr virus,
enteroviruses,
HIV,
Coxsackie, influenza,
hepatitis, mumps,
lymphogranuloma venereum,
rickettsia and variola.
- Bacteria: includes Group A beta haemolytic
streptococcus,
diphtheria, Brucellosis,
mycobacteriae,
Mycoplasma pneumonia
tularemia and
typhoid.
- Fungal: includes
coccidioidomycosis,
dermatophytosis and
histoplasmosis.
- Protozoal: malaria and trichomoniasis.
- Immunisation: associated with immunisation, e.g. measles, hepatitis B.1
- Drug-induced: many drugs have been implicated, e.g. penicillins, sulphonamides,
phenytoin, carbamazepine, non-steroidal anti-inflammatory drugs, anti-malarials
and allopurinol.2
- Cocaine use.
- Radiation therapy for cancer.
- Malignancy: various carcinomas and
lymphomas have been associated.
- Idiopathic: in 25-50% of cases.
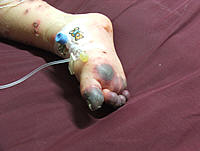
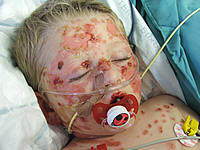
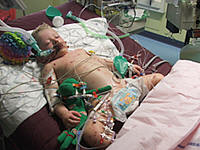
Presentation
Images of typical skin and mucous membrane lesions can be found at the 3 linked
sites listed under Internet and Further Reading below.
- Typically involves the skin and the mucous membranes.
- Minor presentations may occur but presentation may be severe with significant involvement
of mouth, nose, eye, vagina, urethra, gastrointestinal tract and lower respiratory
tract mucous membranes.
- Lesions may continue to erupt in crops for as long as 2-3 weeks.
Symptoms
- Often starts with a non-specific upper respiratory tract infection, which may be
associated with fever, sore throat, chills,
headache, arthralgia, vomiting and
diarrhoea, and malaise.
- Mucocutaneous lesions develop suddenly and clusters of outbreaks last from 2-4 weeks.
The lesions are usually not pruritic.
- Mouth involvement may be severe enough that patients may not be able to eat or drink.
- Respiratory involvement may cause a cough productive of a thick purulent sputum.
- Patients with genitourinary involvement may complain of dysuria or an inability
to pass urine.
Signs
Skin
- General examination: fever, tachycardia, hypotension. Altered level of consciousness,
seizures, coma.
- Lesions may occur anywhere, but most commonly affect the palms, soles, dorsum of
hands and extensor surfaces. The rash may be confined to any one area of the body,
most often the trunk.
- The rash can begin as macules that develop into papules, vesicles, bullae, urticarial
plaques, or confluent erythema.
- The center of the lesions may be vesicular, purpuric, or necrotic.
- The typical lesion has the appearance of a target, which is considered pathognomonic.
- Lesions may become bullous and later rupture. The skin becomes susceptible to secondary
infection.
- Urticarial lesions are usually not pruritic.
- Mucosal involvement: erythema, oedema, sloughing, blistering, ulceration and necrosis.
- Eye: conjunctivitis, corneal ulcerations.
- Genital: erosive
vulvovaginitis or balanitis.
Differential Diagnosis
Investigations
- There are no specific investigations.
- Skin biopsy: demonstrates that the bullae are subepidermal. Epidermal cell necrosis
may be seen and perivascular areas are infiltrated with lymphocytes.
Associated diseases
- Stevens-Johnson syndrome and toxic epidermal necrolysis are variations of the same
disease.
- Toxic epidermal necrosis has a higher mortality (30-35%).3
Erythema multiforme, Stevens-Johnson syndrome and toxic epidermal necrolysis are
differentiated by the extent of epidermal detachment, with greater detachment occurring
in toxic epidermal necrolysis.4
Management
Treatment is supportive:
- Attention to airway and haemodynamic stability.
- Severe fluid loss may require intravenous fluid replacement and electrolyte correction.
- Pain control.
- Skin lesions are treated as burns.
- Mouth: mouthwashes; topical anesthetics are useful in reducing pain and allowing
the patient to take in fluids.
- Management of underlying cause, including identifying and stopping any drug cause.
- Treatment of secondary infection.
- Some have advocated cyclophosphamide, plasmapheresis,
haemodialysis and immunoglobin therapy, but none of those should be considered
standard at this time.3
Immunoglobin therapy has shown the greatest success and is the most widely used.
- The use of systemic
steroids is controversial. Some authors believe that they are contraindicated.
Treatment with systemic steroids has been associated with an increased prevalence
of complications.3
Complications
- Gastrointestinal and respiratory involvement may progress to necrosis.
- Skin: secondary infection and scarring.
- Mucosal pseudomembrane formation may lead to mucosal scarring and loss of function
of the involved organ system.
- Extensive involvement of the oesophagus may cause
oesophageal strictures.
- Lung: mucosal shedding in the tracheobronchial tree may lead to respiratory failure.
- Eye complications: include
corneal ulceration and anterior uveitis. Blindness may develop secondary to
severe keratitis or panophthalmitis in 3-10% of patients.
- Vaginal stenosis and penile scarring have been reported.
- Renal complications are uncommon but
renal tubular necrosis and
renal failure may occur.
Prognosis
- Individual lesions usually heal within 1-2 weeks, unless secondary infection occurs.
- Most patients make a full recovery.
- The prognosis depends on the development of associated serious complications.
- Mortality is 3-15% in patients with severe Stevens-Johnson syndrome.
Prevention
- Future avoidance of any possible or confirmed underlying cause.
Document References
-
Leaute-Labreze C, Lamireau T, Chawki D, et al; Diagnosis, classification, and
management of erythema multiforme and Stevens-Johnson syndrome. Arch Dis Child.
2000 Oct;83(4):347-52. [abstract]
-
Fritsch PO, Sidoroff A; Drug-induced Stevens-Johnson syndrome/toxic epidermal
necrolysis. Am J Clin Dermatol. 2000 Nov-Dec;1(6):349-60. [abstract]
-
Ghislain PD, Roujeau JC; Treatment of severe drug reactions: Stevens-Johnson
syndrome, toxic epidermal necrolysis and hypersensitivity syndrome. Dermatol Online
J. 2002 Jun;8(1):5. [abstract]
-
Bastuji-Garin S, Rzany B, Stern RS, et al; Clinical classification of cases
of toxic epidermal necrolysis, Stevens-Johnson syndrome, and erythema multiforme.
Arch Dermatol. 1993 Jan;129(1):92-6. [abstract]
Internet and Further Reading
Acknowledgements
We are grateful to Dr Colin Tidy for writing this article. The final copy
has passed scrutiny by the independent Mentor GP reviewing team. ©EMIS 2007.
DocID: 2801
Document Version: 20
DocRef: bgp1287
Last Updated: 1 May 2007
Review Date: 30 Apr 2009
WATCH OUT FOR SEPSIS this lead to Joe having complete organ failure and two
years later not being able to cope.